This case series reviews the experiences of three diabetic patients treated at the Intensive Dietary Management clinic in Toronto. All patients were male, ages 40 to 67, with long-term diabetes (10 to 25 years), and all were receiving multiple diabetic medications, including insulin, at baseline. Each patient agreed to follow an intermittent fasting protocol (two patients completed alternating-day 24-hour fasts, while the third followed a triweekly 24-hour fast schedule) in which, in addition to fasting, all meals consumed were directed to be low-carbohydrate to minimize glucose and insulin response. On fasting days, patients only ate dinner; on non-fasting days, they ate lunch and dinner. This protocol was explained during a six-hour nutritional training seminar at study initiation, and patient follow-up visits occurred every two weeks thereafter. Patient 1 followed this diet for seven months, while patients 2 and 3 followed it for 11 months.
The HbA1C responses of patients 1 (40 y/o, T2D for 20 yrs, baseline HbA1C 11), 2 (52 y/o, T2D for 25 yrs, baseline HbA1C 7.2), and 3 (67 y/o, T2D for 10 yrs, baseline HbA1C 6.8) are provided in the figures below.
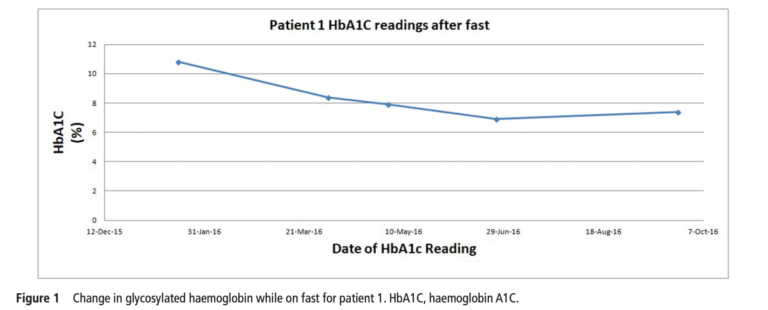
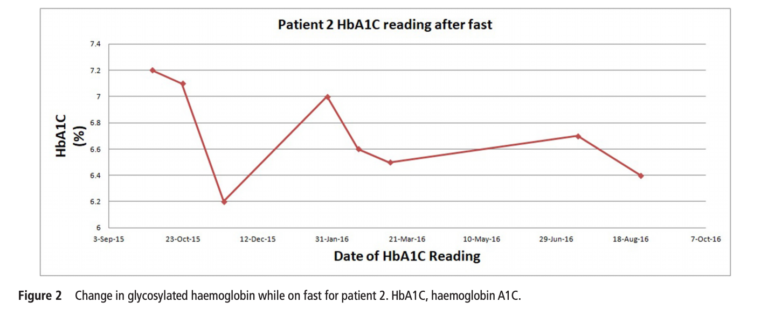
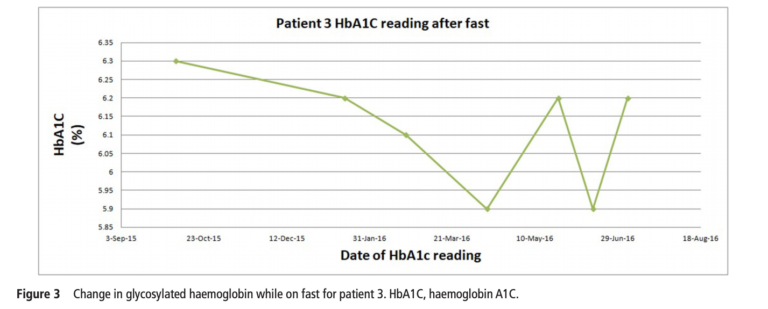 All three patients were able to discontinue insulin less than a month after beginning the regimen, with patient 1 discontinuing insulin five days after therapy began. All patients also saw a decrease in other diabetic medications, with patients 2 and 3 discontinuing all medication and patient 1 discontinuing three out of four medications. HbA1C decreased from 11% to 7%, 7.2% to 6%, and 6.8% to 6.2% in patients 1, 2, and 3, respectively. All patients lost at least 10 kg.
All three patients were able to discontinue insulin less than a month after beginning the regimen, with patient 1 discontinuing insulin five days after therapy began. All patients also saw a decrease in other diabetic medications, with patients 2 and 3 discontinuing all medication and patient 1 discontinuing three out of four medications. HbA1C decreased from 11% to 7%, 7.2% to 6%, and 6.8% to 6.2% in patients 1, 2, and 3, respectively. All patients lost at least 10 kg.
All patients found the diet tolerable and gave positive assessments of how they felt: Patient 1 felt “excellent” on fasting days, patient 2 felt “terrific,” and patient 3 found fasting “easy” and reported higher energy levels.
Overall, the case series illustrated that an intermittent fasting regimen, paired with a low-carbohydrate diet on non-fasting days, can lead to significant improvements in blood glucose levels (as measured by HbA1C) and diabetic condition (as evidenced by the observed reduction in medication), even in long-term diabetics. Future research could build on this by testing different fasting and patient engagement protocols to identify the most efficacious methods for using fasting to control and reverse diabetes.
Comments on Therapeutic fasting as a potential effective treatment for type 2 diabetes
Great. Let's push this non medication solution to this terrible chronic disease.
It's impressive to see such improvements within weeks, even decades after a diabetes diagnosis. Everybody who treats diabetes (type 2) with drugs and everybody who still thinks that diabetes is a chronic progressive disease, should look at these data. There is plenty of evidence that diabetes can be put into remission by dietary interventions (see, for example, the virta health study: https://www.ncbi.nlm.nih.gov/pubmed/31231311). Fasting in combination with a low carb diet may be more efficient than a low carb diet alone, which needs to be tested in randomized trials.
Keeping high quality animal protein up, in combination with resistance training, even in a slight caloric deficit (!) can improve body composition https://www.ncbi.nlm.nih.gov/pubmed/25646324
less fatt & more muscle is a great way to reverse the diabetic phenotype :)
This paper, like the others featured on Crossfit.com, serves a dual purpose. On one hand, it shows the direct benefits of a lifestyle intervention - fasting - on a costly (both in terms of dollars and patient burden) condition - diabetes. At the same time, it also shows in a much broader sense that a condition that has traditionally been treated using drugs or even surgery can instead be rapidly resolved just by changing the diet. I believe this makes a case for the value of lifestyle changes that may have implications far beyond fasting. For example if fasting can lead to these rapid, durable improvements, what about other interventions that also suppress blood glucose and insulin activity, like carbohydrate restriction or intensive exercise programs? If we can develop a suite of interventions for these conditions, and better understand how, when and why each is effective, we may be able to treat with lifestyle with the same ease and confidence we treat with drugs now. I hope to see Fung's team and others in the field continue to build on these results.
Therapeutic fasting as a potential effective treatment for type 2 diabetes
4